How does antibiotic resistance develop?

Our bodies contain countless bacteria. Some of them can be resistant to antibiotics.

Antibiotics kill the bacteria that cause infections as well as the good bacteria.
This allows antibiotic-resistant bacteria to multiply.
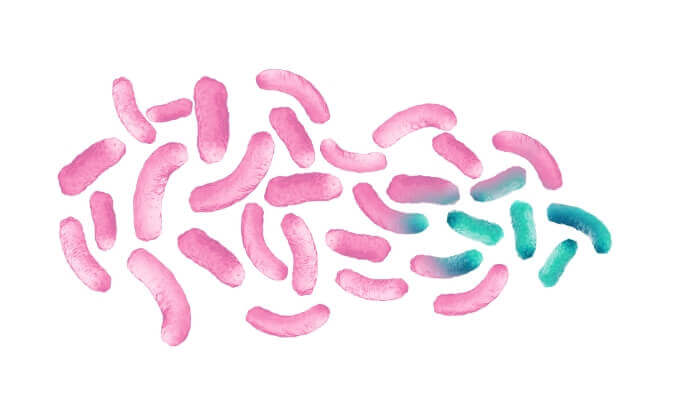
Some bacteria can transmit resistance traits to other bacteria.
In summary
#1
Antibiotic resistance does not mean that the body becomes resistant to antibiotics. It means that bacteria develop the ability to fight off antibiotics designed to eliminate them.
#2
When bacteria become resistant, antibiotics can no longer fight them and the bacteria multiply. These hard-to-treat bacteria can spread and contaminate other people, animals and the environment.
#3
Resistance traits can be passed between different bacteria. It's how some bacteria acquire the ability to resist multiple antibiotics over time.
How does antibiotic resistance spread?
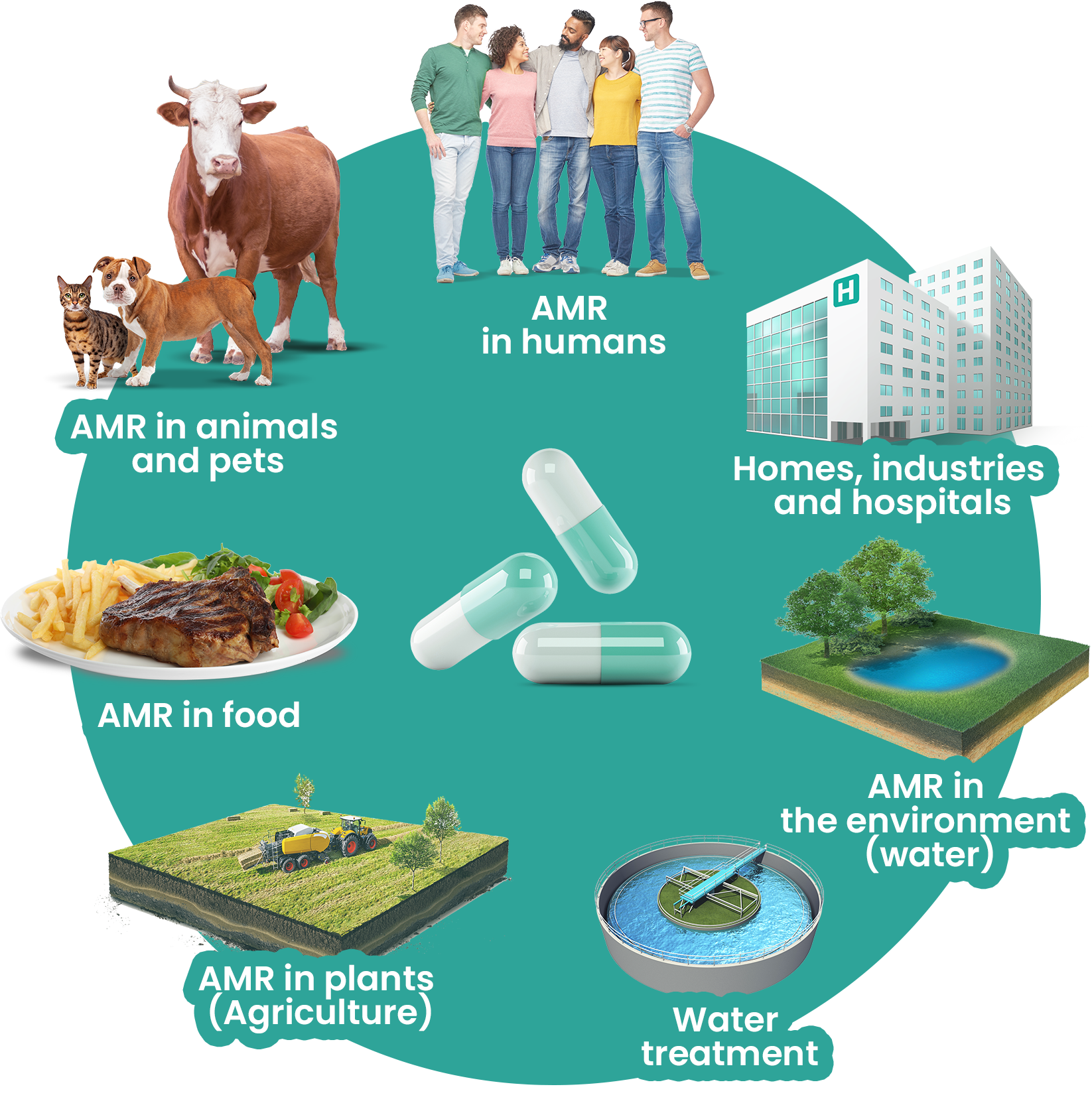
Bacteria are constantly moving between humans, animals and the environment, via simple contact and through food. They are present everywhere: in our homes, hospitals, schools, nursing homes, farms,... Residues of medicines, including antibiotics, and resistant bacteria are also found in the environment, for example in waste water or as a result of inappropriate waste treatment.
This is why AMR needs to be addressed via a “One Health” approach, i.e. an integrated approach to human, animal, plant and environmental health that recognises that human health is linked to animal health, food chain safety and the environment.
Is resistance only a problem with antibiotics?
- Antifungals
- Anti-parasitics
- Antivirals
- Biocides (disinfectants)

